

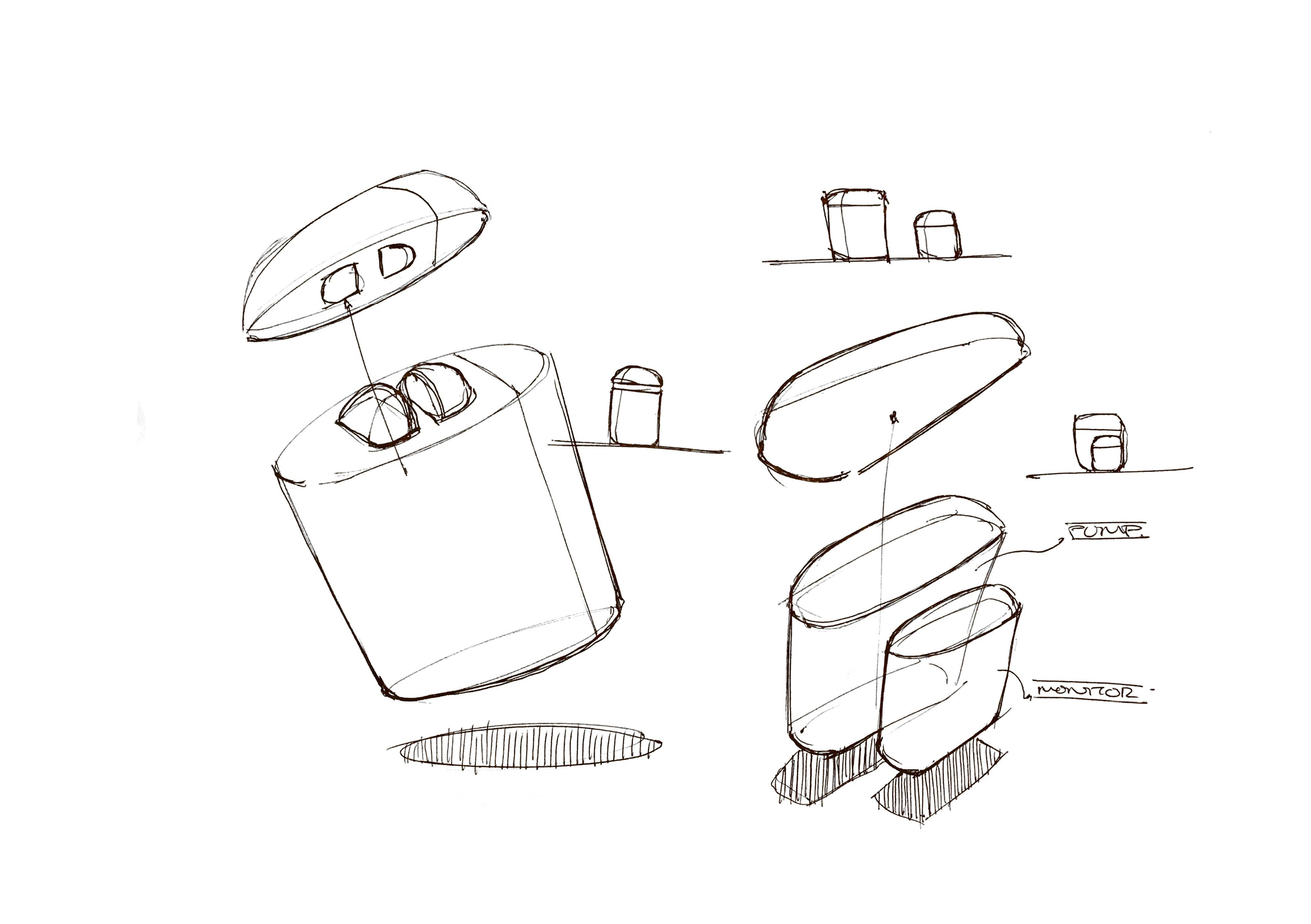

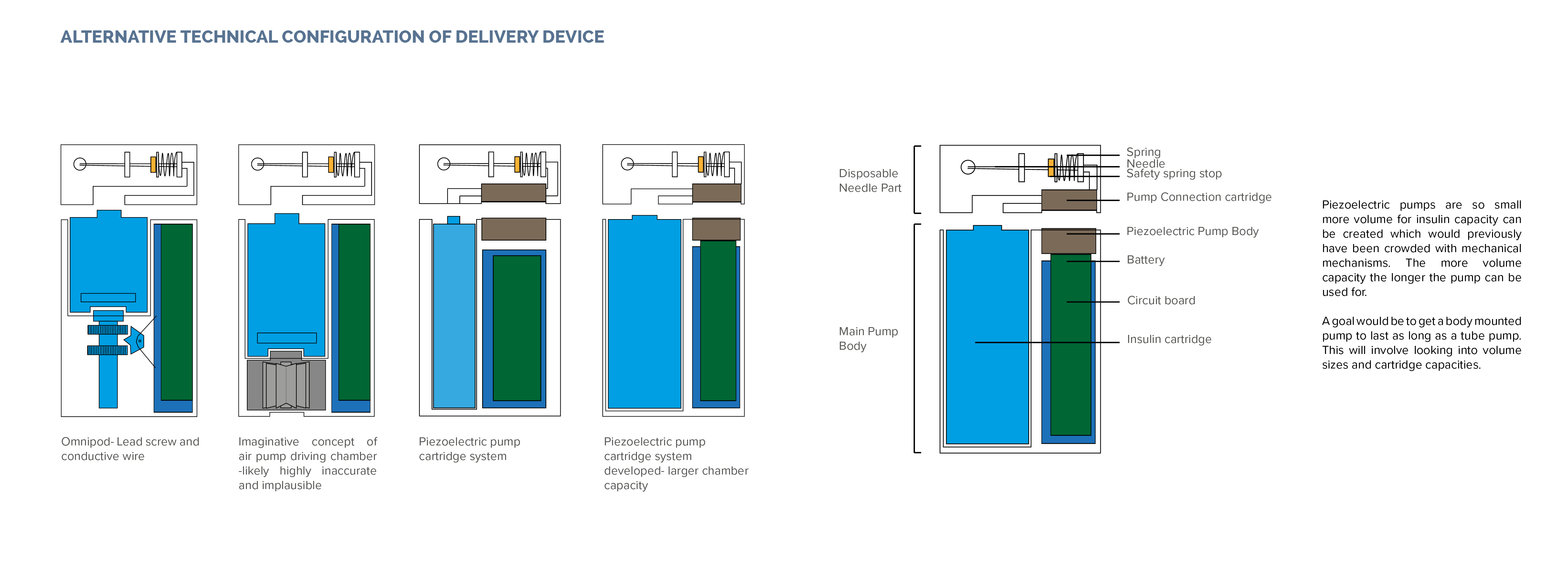
I have been analysing different pump technologies and sterility for transporting the insulin. I have finally decided on the technology and best configuration available. I have been studying different piezoelectric pumps and contacting manufacturers. Using a cartridge based or standard piezoelectric pump in a cartridge form with the needle mounting element all in a disposable part enables the actual pump body to contain a far greater chamber for insulin as well as the battery and circuit board parts. I am now moving on developing the form of the pump thinking more about its appearance and interaction with a charging hub.
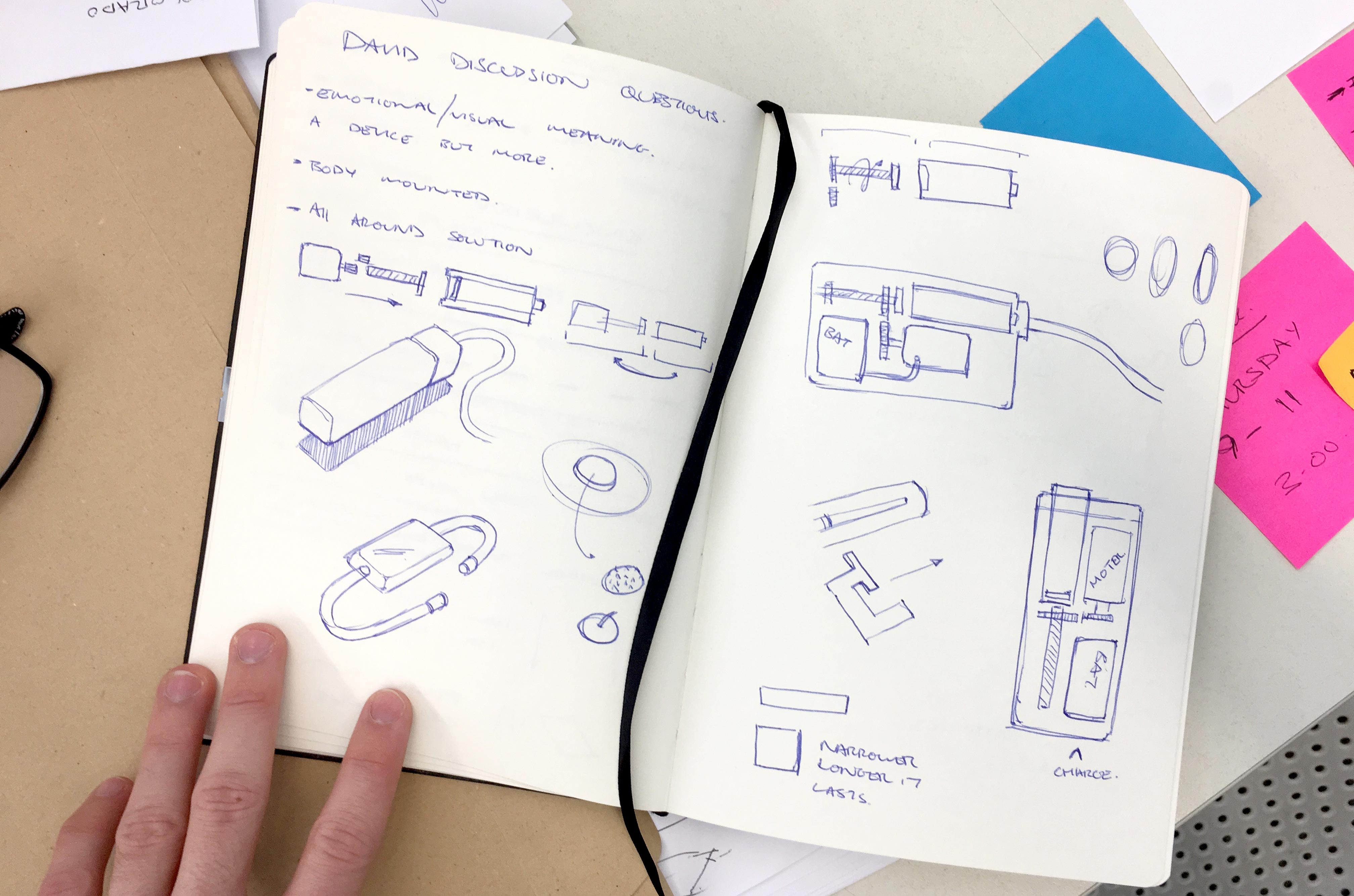
I had been trying to wrap my head around how to make the pump smaller in size. The ‘Omnipod’ is already very small but has limitations in chamber capacity and is disposable. The mechanical ‘lead screw pump system’ is highly compact but wastes space due to the mechanism and need for the same length of chamber in comparison to chamber length. Normal tube pumps function in a similar manner but are driven by a motor rather than a memory wire system therefore they are larger and heavier. I never truly believed a Pump system could be the right approach due to hygienic transfer and movement of the insulin but David convinced me to keep exploring further. We briefly discussed Colgate and their toothpaste pumps.. it would be a case of experiment and explore if it were possible to reengineer a mechanism and think about it functioning in an appropriate manner. I believed I was already reimagining the pump in an innovative manner by using the mechanical principle of the Omnipod but separating and rearranging the components positioning to be insulin and needle cartridge based. To reimagine the pump system inside the device would truly prove a forward driven innovative system.
We also discussed the monitoring device and the balance between a wearable and the pump all acting together as an artificial pancreas for option 5.

Thinking about daily logging and interaction with the provision or monitor device. Developing wireframes considering app interaction and set up stages for the various devices as well as daily logging needs. The main data the app may require to consider for the diabetic is food logging, fitness, glucose level monitoring, pump/insulin provision levels, battery levels of devices, doctor communication.

I attended a lecture on Monday 19th February 2018 by Professor Eric Lars Holmquist (Professor of Innovation).
Professor Holmquist reflected on his past projects and talked about the best ways to produce useful research results. He presented the notion of “grounded innovation” as a strategy for creating new digital products.
The presentation began talking about the ‘Bubble Badge’ a concept he developed in 1998 that prototyped a wearable digital pin badge that was a digital screen. The user could control or program by an external device the information or picture they wished to display and then it could match their fashion sense or beliefs for however long they wished. Holmquist then went onto outline the ‘Drucker’s 5 principle steps of innovation’. 1) searching for opportunity 2) Analysis 3) Listen 4) Focus 5) Leadership. He talked about how the standard innovative product could take up to 20 years for a company to take from concept to final product design and prove its viability in a market opportunity. A key example being touch screen actually invented n 1984 but only truly came into effect – reached the ‘slope of enlightenment’ by companies like Apple in the late 21st century.
He then reverted back to his ‘Bubble Badge’ concept and how in this current day on Kickstarter a similar product is receiving large levels of funding entitled ‘Pins Collective‘ .
A very interesting lecture that motivates an innovative perspective for design.

Very interesting and relevant lecture by Ian Hewitt entitled “Design for Medical and Well Being”
Ian discussed one of the most important considerations when designing medical products which is standards and classifications which are determined by Implant, intrusive and data recording.
There are 3 classes:
Class 1
Class 2
Class 3

Cleaning
Maintenance
Reuse
Consider
Data recording
Diagnosis
Sharps
Materials
End User
Consider constructing DARL and CRL logs as method for development
An incredibly relevant and useful lecture and I have discussed to have a meeting with Ian in the upcoming weeks to gain his thoughts and views on the project.
Had a Spontaneous brief discussion with Neil Smith regarding the project.
As Neil and I had not had a follow up discussion for a while – I realised it was rather complex to briefly explain the status of the project.
After discussing one of the directions Neil bought up some key thoughts that I noted:
“Some people need constant monitoring and adjustable provision others not”
“Could you consider some permission to dial up/ down the pump”
“It comes down to a decision factor regarding viability between one and the other for who you are caring for”
“I used to know people at the university who were 24/7 reliant and it was really important they had appropriate management”
Our meeting was very brief and we plan to follow up later in the week.
 Dr Rachel Clarke quoted a famous Dr William Osler “Just listen to your patient, he is telling you the diagnosis”.
Dr Rachel Clarke quoted a famous Dr William Osler “Just listen to your patient, he is telling you the diagnosis”.
“Stories are important. As a doctor my job is to listen to my patients stories and shape them for the better.
Palliative care doctor (focuses on providing relief from the symptoms, pain, physical stress, and mental stress of a terminal diagnosis. Dr Rachel Clarke specifically specialises in patients at the end of their life)
A very powerful story and example came from The Royal Marsden one of the foremost cancer treatment hospitals where one of the ‘Play specialists’ was trying to make radio therapy less stressful to children. Children face radio therapy for tumours alone inside a radiotherapy machine which is loud and distressing. This can be a challenging and frightening experience for a child or anyone to go through by themselves.
To cope with the challenge the play specialist developed something very simple yet quite ingenious called ‘magic string’ .
The magic string was a ball of twine which could be held at one end by the child/patient and the other end of the thread under the door and by the parent. The play specialist invented a literal story. Narrative thread that enabled the child to tell them selves that even though they were behind a hard lead door and going through the experience themselves they were still being cared for by their mother and father outside the room. A lovely Idea”
Reflection
In terms of Diabetes patients and devices, specifically referring to those first being introduced to the condition, it is particularly important for them to understand the value of connection and support from those close to them as well as others also suffering. For development I must move forward taking into consideration the device monitoring/ provision functionality but also the data recording its meaning and the connection with family members or doctors.